

Business Management
Want content delivered to your inbox?
Suggested Reads for Business Management


Commercial Real Estate Operational Efficiency
Business Management
5 Min Read

Risks of Delaying Business Decisions
Business Management
7 Min Read

Hospitals Partner with Energy Providers to Modernize Infrastructure
Business Management
5 Min Read

Future of AI in Healthcare
Business Management
11 Min Read

How AI Is Reshaping Medicine
Business Management
9 Min Read

How the Continuing Development of Telecom Infrastructure Is Changing the Competitive Landscape
Business Management
6 Min Read

Impact of Middle Market Private Equity
Business Management
5 Min Read

Trends Transforming the Home Building Industry
Business Management
7 Min Read

Private Equity for Gastro and Physical Therapy
Business Management
7 Min Read

7 Steps to a Natural Disaster Business Plan
Business Management
6 Min Read

Sale-Leaseback: Unlock Real Estate Equity
Business Management
9 Min Read

Revolutionize Accounts Payable Webinar
Business Management
2 Min Read

Impacts of AI in Healthcare Real Estate
Business Management
12 Min Read

Real Estate Liquidity for Healthcare Providers
Business Management
5 Min Read

Fee-Fi-Fo-Done with Confusing Banking Charges
Business Management
1 Min Read

Digital Payments Improving Patient Experience
Business Management
5 Min Read

Minority Recapitalization for Your Business
Business Management
7 Min Read

Why Academic Medical Centers Buy Hospitals
Business Management
5 Min Read

How Small, Midsize Companies Prevent Risk
Business Management
9 Min Read

Working Capital for the Self-Employed
Business Management
7 Min Read
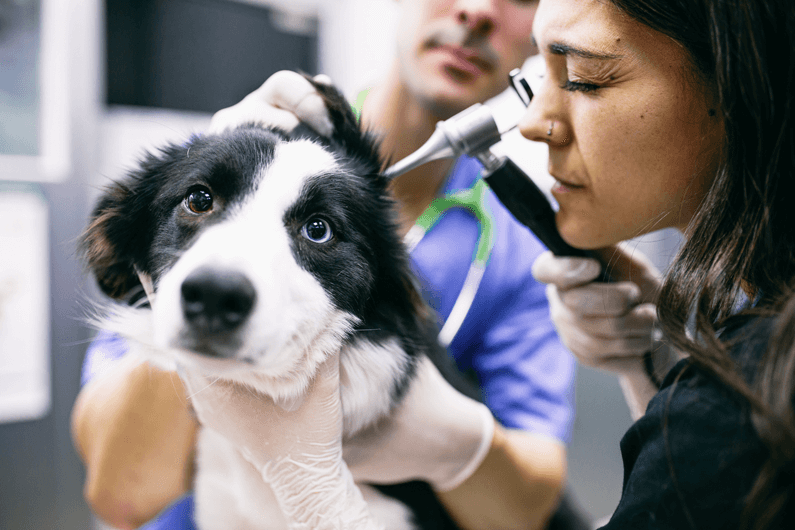
Simplifying Medical Practice Financing
Business Management
5 Min Read

Managing Remote Customer Service Teams
Business Management
6 Min Read

FASB Lease Accounting Rules
Business Management
1 Min Read

Companies Accelerate Digital Transformation
Business Management
6 Min Read

7 Ways to Save Your Business Money
Business Management
5 Min Read

Commercial, Industry Insights
Business Management
6 Min Read

How to Navigate the New Era of Data Regulation
Business Management
5 Min Read

How Businesses Are Reducing Single-Use Plastic
Business Management
5 Min Read

6 Ways to Stay Productive at Work
Business Management
6 Min Read

The Family Business Keys to Success
Business Management
4 Min Read

Steps for Business Continuity in Uneasy Times
Business Management
6 Min Read

Raising Prices: What Small Businesses Can Learn from Big Companies
Business Management
4 Min Read

Have You Outgrown Your Sole Proprietorship?
Business Management
4 Min Read

Making the Gig Economy Work for Your Business
Business Management
5 Min Read

4 Ways Sole Proprietors Can Be More Professional
Business Management
4 Min Read
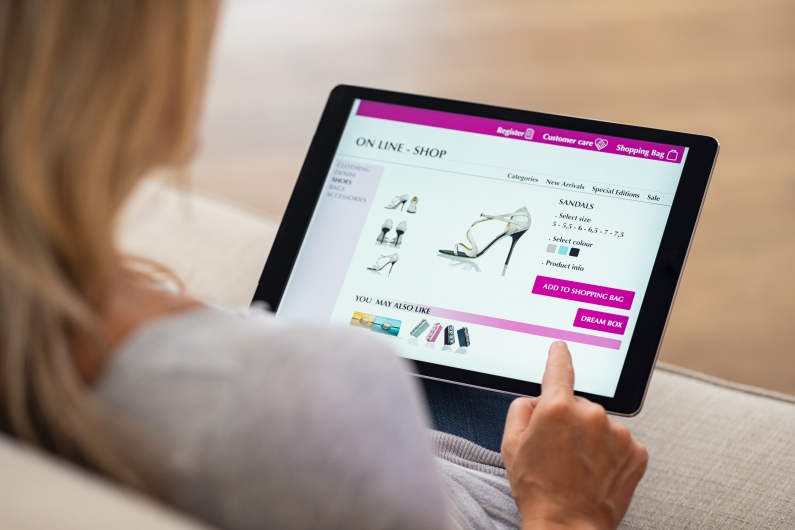
3 Ways to Increase Small Business Ecommerce
Business Management
5 Min Read

3 Signs for Businesses to Raise Their Prices
Business Management
4 Min Read

The Concierge Doctor Will See You, Immediately
Business Management
6 Min Read
Retirement Knowledge Center
Learning about personal finance and reading retirement and investment advice is often times too complex to really understand what needs to be done.
